Can You Be Allergic to Your Partner’s Semen? Understanding Semen Allergy
If sex leaves you with burning, redness, itching, hives, or even swelling “down there,” you might wonder: Am I allergic to my partner’s semen?
It sounds surprising, but semen allergy (also called seminal plasma hypersensitivity) is a real condition that affects some women. Symptoms can range from mild irritation to severe reactions, and it’s often mistaken for infections, irritation, or relationship stress.
This guide covers what semen allergy is, how it shows up, how it’s different from infections like BV or yeast, how to get diagnosed, and practical ways to manage it. It’s not personal medical advice, but it can help you identify whether semen allergy might explain your symptoms and prepare for a productive conversation with your clinician.
What is semen allergy?
Semen allergy happens when your immune system reacts to proteins in a partner’s semen (the fluid that carries sperm).
The reaction is to seminal plasma not sperm itself. Seminal plasma contains:
Proteins from the prostate, seminal vesicles, and bulbourethral glands.
Enzymes, sugars, and other compounds.
Unique to each man (like fingerprints).
Key facts:
Affects an unknown percentage of women (estimates range from 1–6%, possibly underdiagnosed).
Can develop suddenly after years with the same partner, or with new partners.
Can range from mild local irritation to severe systemic reactions.
Unlike latex allergy or spermicide irritation, semen allergy is specifically to partner proteins.
Symptoms of semen allergy
Symptoms usually start minutes to hours after semen contact and can affect:
Local reactions (vulva/vagina)
Burning or stinging inside the vagina or on the vulva.
Redness, swelling, or irritation of vaginal lips.
Itching that worsens after sex.
Hives or rash on genitals or inner thighs.
Deeper vaginal/cervical
Cramping or pelvic discomfort.
Burning during or after sex that feels different from friction.
Watery discharge mixed with irritation.
Systemic (whole body)
Hives or rash spreading to chest, arms, legs.
Swelling of lips, eyelids, or throat (rare but serious).
Shortness of breath or throat tightening (emergency).
Timing clue: Symptoms improve when semen contact is avoided (condoms, no ejaculation inside).
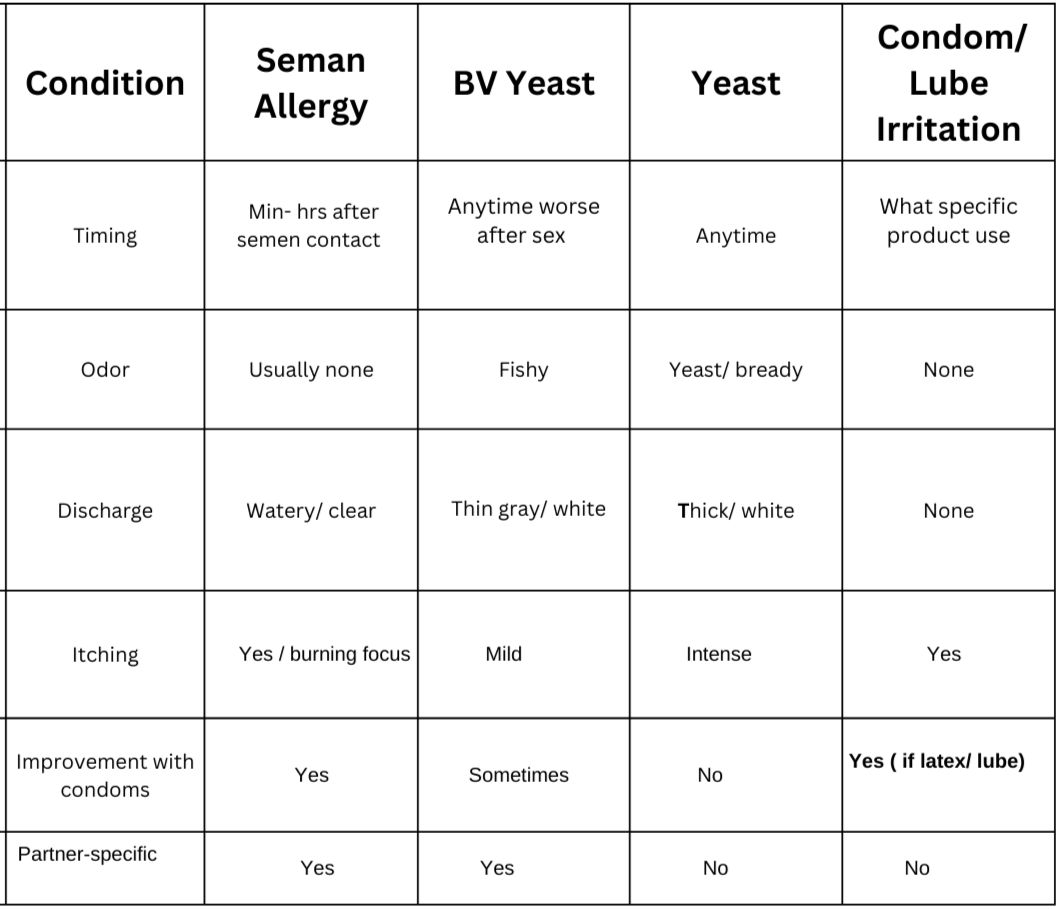
Semen allergy vs infections and irritation
Semen allergy is often mistaken for:
Why does semen allergy happen?
Your immune system mistakes harmless semen proteins for threats, producing:
IgE antibodies (immediate allergic reaction).
IgG antibodies (delayed reaction).
Histamine and inflammatory chemicals.
Possible triggers:
New partner (different proteins).
Pregnancy/hormones changing immune response.
Past exposure sensitizing the immune system.
Genetic predisposition to allergies.
Rare but serious: Postorgasmic illness syndrome in men (symptoms after their ejaculation) suggests bidirectional reactions.
How to get diagnosed
Self‑diagnosis is impossible symptoms overlap too much. Diagnosis involves:
Detailed history
Timing of symptoms (after unprotected sex?).
Partner‑specific (same partner years, then sudden onset?).
Improvement with condoms/no ejaculation.
Past allergies or autoimmune issues.
Rule out infections
Swabs for BV, yeast, trichomoniasis, STIs.
Urine culture for UTIs.
Allergy testing rarely done (no standard semen allergy test).
Provocation test (research setting)
Condom sex (no reaction) → unprotected ejaculation (reaction confirms).
Not routine risky and uncomfortable.
Diagnosis of exclusion: Symptoms fit pattern + infections ruled out + improve with semen avoidance.
Managing semen allergy
Once diagnosed (or strongly suspected), options include:
Primary strategy: Avoid semen contact
Condoms for all vaginal/anal sex.
Withdrawal/no ejaculation inside vagina.
Non‑penetrative intimacy.
Pro tip: Discuss with partner early frame as health issue, not rejection.
Desensitization (rare)
Partner immunotherapy: Diluted semen samples given vaginally over months.
Experimental, specialist‑only.
Variable success, time‑intensive.
Symptom relief
Topical steroids/creams for irritation (short‑term).
Antihistamines for systemic reactions (consult clinician).
Cool compresses for burning/swelling.
Emergency: EpiPen if anaphylaxis history.
Partner considerations
For your partner:
Not their “fault” proteins are unique, not hygiene.
No treatment needed (they’re asymptomatic).
Condoms protect both (STI prevention).
Relationship impact:
Early, blame‑free communication key.
Explore non‑ejaculatory intimacy.
Couples therapy if intimacy stress builds.
Frequently asked questions
Q: Can semen allergy develop suddenly?
Yes. Can appear after years with same partner due to immune changes, pregnancy, stress.
Q: Is it the same as latex allergy?
No. Latex allergy reacts to condom material. Semen allergy is partner‑specific proteins. Can have both.
Q: Does birth control affect it?
Hormonal changes (pills, IUD, pregnancy) may influence immune response and symptom severity.
Q: Can I still get pregnant with semen allergy?
Yes, via:
Condoms until ovulation window.
Withdrawal + fertility tracking.
IUI/IVF if severe.
Discuss with fertility specialist.
Q: Is semen allergy permanent?
Possibly, but some desensitize over time or with treatment. Many manage successfully long‑term.
Q: Does this mean I can’t have sex?
No condoms, withdrawal, non‑penetrative options work for most couples.
Key takeaways
Semen allergy is real but often underdiagnosed burning, hives, swelling after unprotected sex are red flags.
Partner‑specific, improves with semen avoidance (condoms).
Rule out infections first BV, yeast, STIs mimic it.
Open partner communication + clinician guidance = best outcomes.
If unprotected sex consistently causes genital burning/hives that resolve with condoms, print this and take to your clinician. You deserve answers beyond “it’s probably just irritation.”
About the Author
Becky Freeman is the founder of BVTalks® and Bee Vee Clean. She focuses on women’s intimate health, vaginal microbiome education, and creating practical, easy-to-understand content for everyday care.
Medical Disclaimer
This content is for educational purposes only and is not intended to diagnose, treat, cure, or prevent any condition. It should not be used as a substitute for professional medical advice, diagnosis, or treatment. Always consult a licensed healthcare provider if you have questions about your health or symptoms.