Perimenopause: The Silent Years You Were Never Warned About
“Women in their 40s sharing conversation
Perimenopause the years leading up to menopause is often called the "silent years" because symptoms sneak up gradually, starting as early as your mid-30s and lasting 4–10 years (average 4–8). Unlike menopause (defined as 12 months without periods), perimenopause brings wild hormone fluctuations declining estrogen, erratic progesterone, rising FSH that affect everything from cycles to vaginal health.
For BVTalks readers dealing with BV or vaginal symptoms, perimenopause can amplify issues like odor, dryness, and recurrent infections. This comprehensive guide covers the four stages, key symptoms (especially vaginal/pelvic), management options, and when to seek care.
The Four Stages of Perimenopause
Perimenopause unfolds in phases, each with distinct changes: MyMenopauseCentre
Average end: Age 51 (range 45–55). Future-Women Evernow
Common Perimenopause Symptoms by Category
Cycle & Bleeding Changes (90% affected)
Irregular periods: Shorter/longer, heavier/lighter, spotting.
Flooding: Heavy flow (soaks pad hourly).
Skipped cycles: 60+ days amenorrhea signals late stage.
Vaginal tie‑in: Heavier flow raises infection risk (BV).
Vasomotor Symptoms (75–85%)
Hot flashes: Sudden heat waves, sweating, heart racing (day/night).
Night sweats: Soaking sheets, insomnia.
Duration: 7–10 years average.
Vaginal & Pelvic Changes (50–70%)
Estrogen decline causes genitourinary syndrome of menopause (GSM) thinning vaginal tissue, rising pH (4.5+), mimicking BV vulnerability.
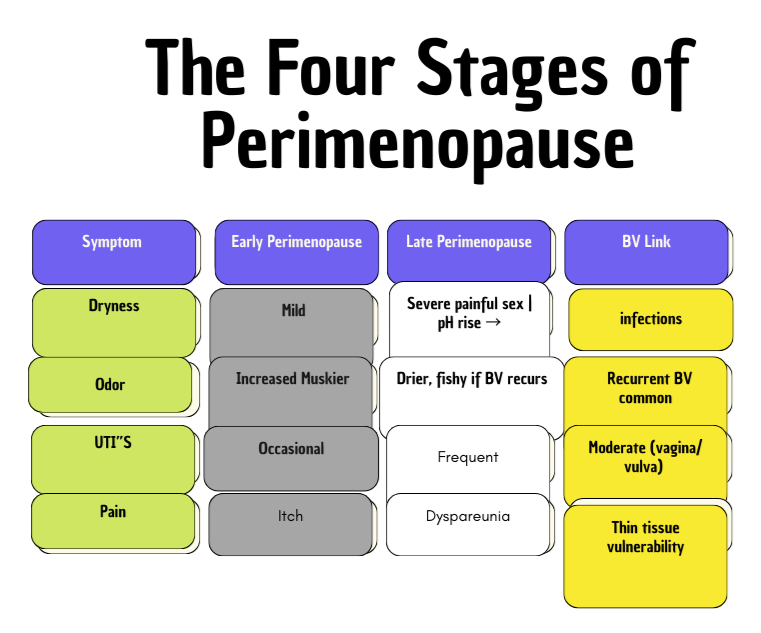
**Early Perimenopause:**
• Dryness: Mild
• Odor: Increased, muskier
• UTIs: Occasional
• Pain: Itch
**Late Perimenopause:**
• Dryness: Severe, painful sex
• Odor: Drier, fishy if BV recurs
• UTIs: Frequent
• Pain: Dyspareunia
Timeline: Worsens late perimenopause.
Mood, Brain & Sleep (60–80%)
Irritability/anxiety: Hormone swings.
Brain fog: Memory/concentration lapses.
Insomnia: Night sweats + anxiety.
Physical Changes
Weight gain (estrogen → fat storage).
Joint pain/fatigue.
Hair/skin thinning.
Vaginal Health in Perimenopause: Deep Dive
Estrogen's role: Keeps vaginal epithelium thick, glycogen‑rich (feeds Lactobacillus), pH acidic. Decline → atrophic changes:
Tissue thins → microtears → infections.
pH rises → BV/yeast risk x2–3.
Discharge decreases → concentrated odor.
BV overlap: Perimenopause women have 30–50% higher BV rates; test recurrent fishy odor.
Management tiers:
Non‑hormonal: Hyaluronic acid moisturizers, DHEA suppositories.
Hormonal: Low‑dose vaginal estrogen (rings/creams).
Lifestyle: Pelvic floor Kegels, phytoestrogens (soy).
Diagnosis: Confirming Perimenopause
No single test, but:
FSH/AMH (elevated FSH >30 IU/L).
Cycle tracking (60+ days amenorrhea).
Symptom diary + antimüllerian hormone.
Rule out thyroid/PID (overlap).
Management by Symptom
Cycle Control
NSAIDs/tranexamic acid for heavy bleeding.
Mirena IUD (progestin stabilizes).
Hot Flashes
Cognitive behavioral therapy (CBT).
SSRIs (paroxetine low‑dose).
Avoid triggers (spicy, caffeine).
Vaginal Dryness/BV Risk
Moisturizers 2–3x/week.
Probiotics post‑antibiotics.
Condoms if semen triggers BV.
Mood/Sleep
Exercise 150 min/week.
Melatonin/magnesium.
When to Seek Care Urgently
Heavy bleeding (soaks pad hourly).
PID symptoms (fever, pelvic pain).
Depression worsening.
12 months no period = menopause confirmed.
Frequently Asked Questions
Q: Perimenopause = menopause?
No. Peri = transition (irregular cycles). Menopause = 12 months amenorrhea.
Q: Can perimenopause cause BV recurrence?
Yes rising pH mimics BV vulnerability. Test odor changes.
Q: HRT safe in perimenopause?
Low‑dose vaginal yes; systemic weighs risks/benefits.
Q: Average age?
Starts 45–47, ends 51 (range 40–55).
Takeaway: Perimenopause vaginal changes amplify BV risk test symptoms, moisturize, track cycles. Print for clinician.
References:
About the Author
Becky Freeman is the founder of BVTalks® and Bee Vee Clean. She focuses on women’s intimate health, vaginal microbiome education, and creating practical, easy-to-understand content for everyday care.
Medical Disclaimer
This content is for educational purposes only and is not intended to diagnose, treat, cure, or prevent any condition. It should not be used as a substitute for professional medical advice, diagnosis, or treatment. Always consult a licensed healthcare provider if you have questions about your health or symptoms.