Hidradenitis Suppurativa Stages and Severity: Mild, Moderate, or Severe?
Hidradenitis Suppurativa Stages: Mild, Moderate, or Severe?
Once you finally hear “hidradenitis suppurativa” (HS) instead of “ingrown hairs” or “recurrent boils,” the next question is usually: “How bad is it and can it get worse?”
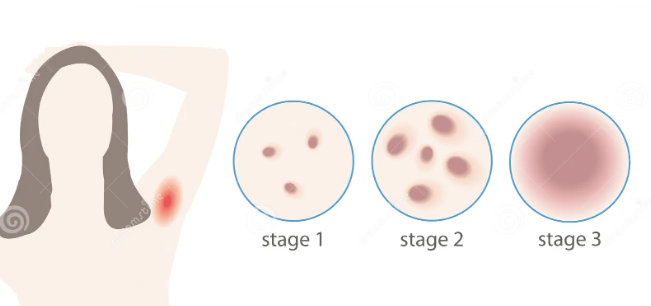
Doctors answer that with staging systems. The most widely used is the Hurley system, which groups HS into mild (Stage 1), moderate (Stage 2), and severe (Stage 3) based on how many areas are involved, whether there are tunnels (sinus tracts), and how extensive scarring has become. Understanding your stage can help you make sense of your symptoms, advocate for stronger treatment if needed, and track whether things are improving. dermnetnz+2
Why HS Is Staged
HS is a chronic inflammatory disease of the hair follicles in skin‑fold areas: armpits, groin, vulva, buttocks, under the breasts, and more. It tends to progress over time if it’s not treated aggressively enough: ncbi.nlm.nih+1
At first, you might see isolated boils that come and go.
Later, lesions can return in the same spots, connect under the skin, and leave ropey scars.
In severe cases, whole regions can become a map of tunnels, scars, and open wounds. metrobostoncp+1
Staging systems like Hurley or more detailed scores (IHS4, HASI‑R, HiSQOL) give clinicians a shared language to:
Decide whether your HS is mild, moderate, or severe.
Choose treatments strong enough for your situation.
Document whether therapies are actually helping over time. hsdiseasesource
For this post, we’ll stick to the Hurley stages because they’re what most patients hear in real‑life appointments.
Hurley Stage 1: Mild HS
What it looks like
Hurley Stage 1 is considered mild disease, but “mild” is misleading; these lesions can still hurt like hell.
Typical features:
Single or a few painful lumps (nodules or abscesses) in classic HS areas: armpits, groin, vulva, inner thighs, buttocks, under breasts. dermnetnz
Lesions may look like deep cystic acne or “boils.”
They heal between flares and don’t yet leave dramatic scars or tunnels.
There are no sinus tracts (no deep channels connecting lumps under the skin). dermnetnz
Many people in Stage 1 are told they just have ingrown hairs, folliculitis, or “sensitive skin,” especially in the bikini area, and may bounce between urgent care visits and short antibiotic courses. hsdisease
How it feels
Pain can range from sore and throbbing to sharp, stabbing pain with movement.
Flares often show up around periods, after shaving, or with heat/friction.
You may feel self‑conscious about swelling and occasional drainage but can often still exercise, work, and have sex, even if it hurts. nhs
Why early Stage 1 matters
Stage 1 is when early treatment can actually change the trajectory of HS:
If you catch it now, topical treatments, short courses of oral antibiotics, and lifestyle changes may prevent progression. pmc.ncbi.nlm.nih
Weight reduction and smoking cessation at this stage are associated with fewer new lesions and slower disease progression. ncbi.nlm.nih
Dermatology guidelines emphasize that Stage 1 is not “too mild” to treat, especially in intimate areas like the vulva or groin.
Hurley Stage 2: Moderate HS
Is where HS crosses the line from “bad breakouts” to true chronic disease.
What it looks like
You still have abscesses and nodules, but now they are recurrent and often in multiple spots.
You start to develop sinus tracts tunnels under the skin that connect lesions. These may open as little holes that leak pus or blood. metrobostoncp
There’s visible scarring: thick lines, ropey ridges, or puckered areas where past lesions healed.
Lesions are usually “widely separated” rather than forming one giant confluent area; you might have several involved patches in the groin, under the breasts, or between the buttocks. hsdiseasesource
You might notice that as soon as one bump heals, another appears nearby, or that the area never feels truly normal anymore.
How it feels
Pain is often daily at this point tender lumps and throbbing tunnels that flare with movement, sweat, or tight clothes.
Drainage can be constant or on‑and‑off, causing worry about odor, staining clothes, and leaking through pads or underwear. vulvovaginaldisorders
Sex, exercise, and sitting may now be significantly limited by pain, especially with groin or vulvar HS. healthline]
Emotionally, Stage 2 is often when people realize “this isn’t going away on its own” and start searching for an HS specialist.
Why Stage 2 is a turning point
This stage is still very treatable, but topical treatments alone are rarely enough. pmc.ncbi.nlm.nih]
Guidelines usually recommend systemic therapy now oral antibiotics for several months, hormonal therapy for some women, and often biologics (like adalimumab) if disease is active and scarring is starting.
Because tunneling has begun, early surgical options such as deroofing individual sinus tracts can prevent larger, interconnected networks from forming.
If you’ve been labeled “moderate HS” or “Hurley Stage 2” and are still only getting creams or occasional I&Ds, that’s a sign to talk about stepping up treatment.
Hurley Stage 3: Severe HS
Is the most advanced, severe form of HS and can be truly disabling.
What it looks like
Large regions entire armpits, groins, buttocks, or under‑breast areas are involved all at once.
There are multiple interconnected sinus tracts and abscesses across the whole area, with little or no normal skin between lesions.
Scarring is extensive, with thick bands, contractures, and sometimes distortion of normal anatomy (for example, in the vulvar and perineal region).
Flares can extend over large body surface areas, and new lesions appear frequently.
How it feels
Pain is often severe, constant, and deep, frequently rated as one of the most painful chronic skin conditions.
Movement walking, lifting arms, sitting, or sex can be excruciating. Some people require disability leave or mobility aids because of HS.
Drainage can be heavy and persistent, leading to chronic skin maceration, odor, and repeated secondary infections. vulvovaginaldisorders
Stage 3 disease is also linked with higher risks of anemia, depression, metabolic syndrome, and rarely squamous cell carcinoma in long‑standing lesions.
Treatment at Stage 3
Biologic therapies (like adalimumab and other targeted immune medications) are usually first‑line systemic treatments.
Combination therapy with antibiotics, intralesional steroids, and sometimes hormonal medications is common.
Surgery is often necessary wide excisions to remove entire affected areas, sometimes followed by grafts or flaps.
Pain management, mental health support, and occupational/physical therapy are crucial parts of care. vulvovaginaldisorders
Even in Stage 3, people can experience dramatic improvements with the right team and aggressive treatment but the goal is to prevent people from ever reaching this stage.
Other Ways Doctors Measure HS Severity
Hurley staging is simple and widely used, but it doesn’t capture day‑to‑day symptoms or quality of life. Newer tools add more nuance:
IHS4 (International HS Severity Score System): counts nodules, abscesses, and draining tunnels to give a numeric severity score; a 55% drop (IHS4‑55) is often used to define treatment response.
HASI‑R and HS‑IGA: standardized ways to grade inflammation, body areas involved, and lesion types, often used in clinical trials.
HiSQOL: a patient‑reported questionnaire that captures pain, psychosocial impact, and day‑to‑day adaptations; higher scores mean more severe impact. ott.psu
You may see these terms in research articles or specialty clinics, but for most appointments, your dermatologist will still say “Hurley Stage 1, 2, or 3.”
Can HS Move From One Stage to Another?
Yes, HS can progress or improve over time, depending on several factors:
Things that push HS toward more severe stages:
Delayed diagnosis and years of treating “boils” without addressing HS.
No systemic therapy when stage 2 disease is clearly present.
Ongoing smoking or uncontrolled metabolic syndrome.
Mechanical friction from tight clothing, certain jobs, or chronic moisture.
Things that help keep HS milder or move it toward remission:
Early diagnosis, ideally in Stage 1.
Lifestyle changes: stopping smoking, gentle weight reduction, minimizing friction.
Appropriate use of biologic therapies and/or surgery when indicated.
Consistent follow‑up with a dermatologist who actually knows HS.
Staging is not destiny; it’s a snapshot of where your disease is right now, and treatment choices can shift that picture over time.
How to Talk to Your Doctor About HS Severity
If you suspect HS or already have a diagnosis, you can use staging language to push for the care you need.
Examples:
“I’ve been told I have HS. I have recurrent abscesses in my groin with tunnels and some scarring. That sounds like Hurley Stage 2. Are we using treatments strong enough for that level of disease?”
“My groin and buttocks are almost fully covered with interconnected tracts and draining lesions. That sounds like Stage 3 HS. Can we talk about biologics and referral to an HS center?”
“Right now I have single nodules that come and go with no scarring. I think I’m Stage 1. What can we do to prevent progression to Stage 2?”
If your clinician seems unfamiliar with HS staging or downplays your symptoms, it’s reasonable to ask for referral to a dermatologist, especially one who participates in HS research or specialty clinics.
Key Takeaways
The Hurley system divides HS into three stages:
Stage 1 (mild): recurrent nodules or abscesses, no tunnels or scarring.
Stage 2 (moderate): recurrent lesions plus sinus tracts and scarring, often in multiple, separated areas.
Stage 3 (severe): diffuse involvement with many interconnected tunnels, scars, and abscesses across an entire region.
FAQ
What Are the 3 Stages of Hidradenitis Suppurativa?
The stage depends on:
Frequency of flare-ups
Presence of scarring
Formation of tunnels under the skin
How widespread the lesions are
If you’re noticing recurring nodules in the same area with scarring or drainage, that may suggest Stage 2 or Stage 3.
A healthcare provider can properly assess severity and determine the correct stage.
Does Hidradenitis Suppurativa Get Worse Over Time?
HS does not automatically progress, but without proper management it can worsen.
Some people remain in Stage 1 for years. Others experience progression if flare-ups are frequent and inflammation remains uncontrolled.
Early diagnosis and treatment can help reduce progression and minimize long-term scarring.
Staging helps determine how aggressive treatment should be and whether you should be offered systemic medications, biologics, and/or surgery, not just creams and occasional drainage.
HS can progress without proper care, but early diagnosis, lifestyle changes, and modern therapies can keep it from advancing and, in many cases, push it toward remission.
Knowing your HS stage isn’t about labeling you it’s about getting the right level of help. If your “ingrown hairs” keep coming back in the same places, or you’re already seeing tunnels and scars, you’re not being dramatic; you’re dealing with a real, chronic disease that deserves serious treatment.
About the Author
Becky Freeman is the founder of BVTalks® and Bee Vee Clean. She focuses on women’s intimate health, vaginal microbiome education, and creating practical, easy-to-understand content for everyday care.
Medical Disclaimer
This content is for educational purposes only and is not intended to diagnose, treat, cure, or prevent any condition. It should not be used as a substitute for professional medical advice, diagnosis, or treatment. Always consult a licensed healthcare provider if you have questions about your health or symptoms.