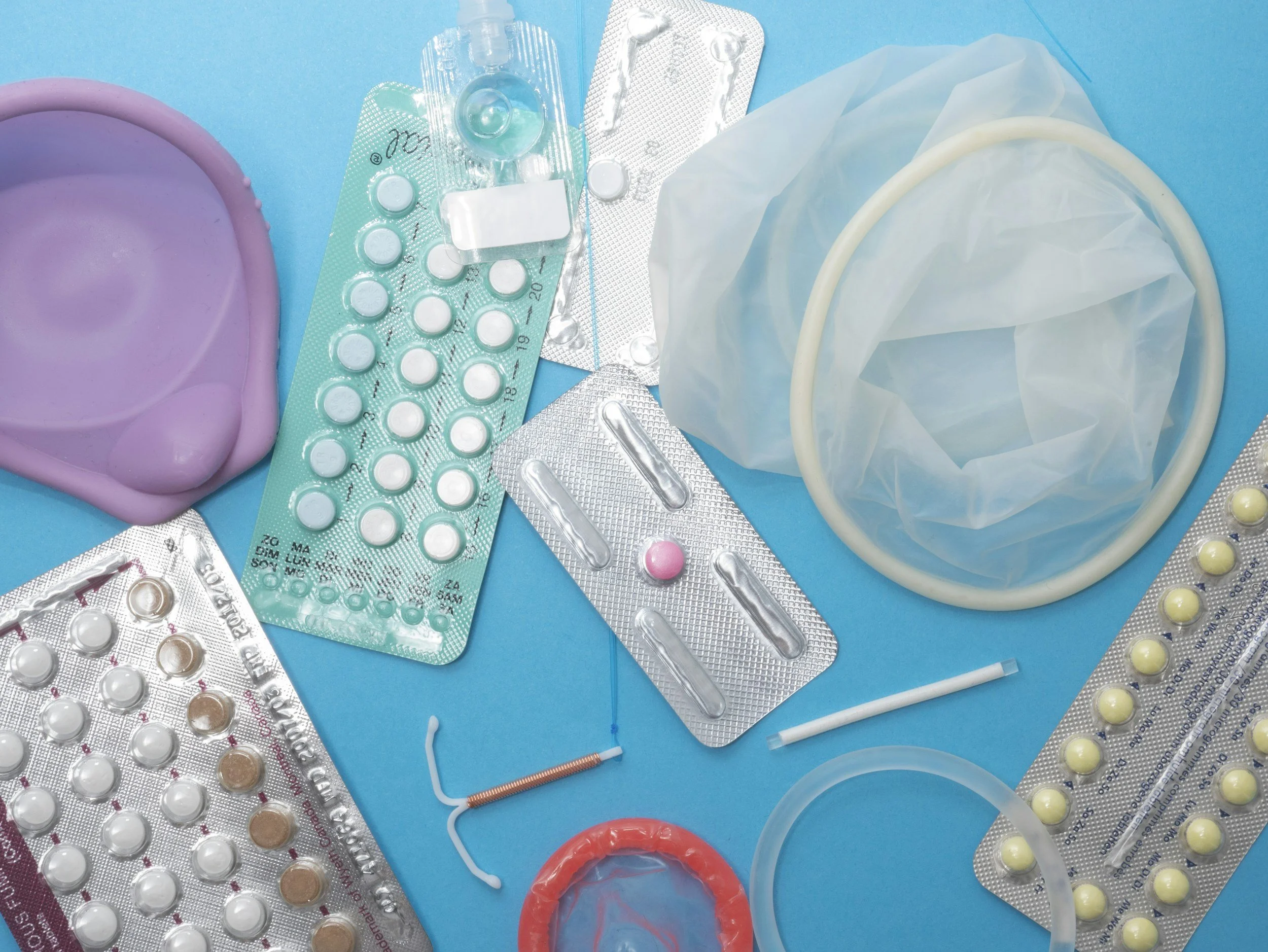
Birth Control Side Effects Nobody Prepares You For
You walk into your doctor's office at 19, 25, or 32 years old and walk out with a prescription for the pill, a shot, an implant, or an IUD. You're handed a folded pamphlet the size of a road map, told the most common side effects are nausea and spotting, and sent on your way.
What that pamphlet doesn't tell you and what your doctor often doesn't have time to explain is that hormonal birth control can affect nearly every system in your body. Your mood. Your libido. Your vaginal pH. Your gut. Your skin. Your ability to absorb certain nutrients. Your risk of recurring infections.
None of this means birth control is bad or that you shouldn't use it. Millions of women use it safely and effectively every day. But informed consent means knowing the full picture not just the highlights so you can recognize what's happening in your body, advocate for yourself, and make the choices that are right for you.
This is the post your doctor's office should have given you.
How Hormonal Birth Control Works
Before diving into side effects, a quick foundation: most hormonal birth control works by delivering synthetic versions of estrogen, progesterone, or both. These synthetic hormones prevent pregnancy primarily by:
Suppressing ovulation stopping the ovaries from releasing an egg
Thickening cervical mucus making it harder for sperm to reach an egg
Thinning the uterine lining making implantation less likely if fertilization did occur
The different types of hormonal birth control include:
Combined oral contraceptive pill (COC) contains synthetic estrogen and progestin
Progestin-only pill (mini-pill) contains only synthetic progestin
Hormonal IUD (Mirena, Kyleena, Liletta, Skyla) releases low-dose progestin locally in the uterus
The implant (Nexplanon) a small rod inserted under the skin of the upper arm; releases progestin
The shot (Depo-Provera) progestin injection given every 3 months
The patch and vaginal ring (NuvaRing) combined estrogen and progestin, delivered transdermally or vaginally
Each method delivers hormones differently, at different doses, and with different systemic effects. This matters because not all birth control side effects are the same across all methods and switching methods can sometimes resolve issues that seem unsolvable.
The Side Effects Nobody Warns You About
1. Mood Changes, Anxiety, and Depression
This is perhaps the most widely experienced yet most minimized birth control side effect. Women have been reporting mood changes on hormonal birth control for decades and being dismissed by providers for almost as long.
The science is catching up. A landmark 2016 Danish study published in JAMA Psychiatry which followed over one million women for 13 years found that women using combined hormonal contraceptives were 80% more likely to be prescribed antidepressants than non-users. For adolescents on the pill, the risk was even higher.
Progestin, the synthetic progesterone used in most hormonal birth control, can affect serotonin and GABA receptors in the brain the same receptors targeted by antidepressants and anti-anxiety medications. Different progestin types (levonorgestrel, drospirenone, norethindrone, desogestrel) have varying effects on mood, which is why switching pill formulations sometimes helps.
What to watch for: persistent low mood, emotional flatness or "numbness," increased anxiety, irritability, crying without clear cause, or loss of enjoyment in things that used to make you happy.
2. Loss of Libido
If your sex drive has dropped significantly since starting hormonal birth control, you are far from alone and you are not imagining it.
The pill, in particular, increases levels of sex hormone-binding globulin (SHBG) in the blood. SHBG binds to testosterone, making it unavailable for use by the body. Since testosterone plays a key role in sexual desire for women as well as men, elevated SHBG effectively lowers your functional testosterone levels sometimes dramatically.
Research published in the Journal of Sexual Medicine found that women on the combined pill had significantly higher SHBG levels and lower free testosterone than non-users and that in some women, SHBG levels remained elevated even after stopping the pill, sometimes for months. This may explain why some women experience persistent low libido even after discontinuing birth control.
What to watch for: significantly reduced interest in sex, difficulty becoming aroused, reduced sensitivity, or changes in orgasm intensity.
3. Vaginal Dryness and Changes in Discharge
Hormonal birth control particularly the pill can cause vaginal dryness and changes in cervical mucus that many women mistake for other conditions. By suppressing natural estrogen fluctuations, the pill can reduce vaginal lubrication, making sex uncomfortable or even painful.
The progestin in hormonal contraceptives also thickens cervical mucus which is part of how it prevents pregnancy, but also means your natural vaginal discharge may look and feel different than it did before. Some women notice less discharge overall; others notice it becomes thicker or changes texture throughout the month.
What to watch for: dryness or discomfort during sex, significant reduction in vaginal discharge, or discharge that seems unusually thick or scant.
4. Disruption of Vaginal pH and Increased BV Risk
This one connects directly back to the BVTalks community: hormonal birth control can alter your vaginal pH and microbiome, increasing susceptibility to bacterial vaginosis and yeast infections.
Estrogen plays a critical role in maintaining Lactobacillus dominance in the vagina. When synthetic hormones suppress your natural estrogen fluctuations or when progestin-only methods lower estrogen below its normal range the vaginal environment becomes less hospitable to the protective Lactobacillus bacteria that keep BV-causing organisms in check.
Several studies have found associations between hormonal contraceptive use and:
Increased rates of BV particularly with progestin-only methods and the hormonal IUD
Altered vaginal microbiome composition reduced Lactobacillus dominance and increased microbial diversity (which in vaginal health terms means more disruption)
Increased yeast infections particularly on the combined pill, due to elevated glycogen in vaginal cells that feeds Candida
If your BV or yeast infections started or worsened after beginning a hormonal contraceptive, this connection is worth discussing with your provider.
What to watch for: new or worsening BV or yeast infections after starting birth control, unusual odor, or discharge changes that align with your contraceptive start date.
5. Nutrient Depletion
This is one of the least-discussed birth control side effects, yet it has wide-ranging implications for energy, mood, immunity, and overall health. Research has shown that long-term use of the combined oral contraceptive pill is associated with depleted levels of several key nutrients:
Folate (B9) critical for cell production and especially important if you plan to become pregnant; pill users may need higher supplementation
Vitamin B6 involved in serotonin production; depletion may contribute to depression and mood changes on the pill
Vitamin B12 essential for nerve function and energy; lower levels linked to fatigue and brain fog
Magnesium involved in over 300 enzymatic reactions; low magnesium is associated with worse period pain, sleep problems, anxiety, and muscle cramps
Zinc important for immune function, skin health, and hormone production
Vitamin C and E antioxidant vitamins that may be depleted with long-term pill use
This does not mean the pill is dangerous. It means that women on long-term hormonal birth control may benefit from targeted supplementation and regular nutritional blood work something most prescribers never mention.
What to watch for: persistent fatigue, brain fog, frequent illness, mood changes, muscle cramps, or hair loss all of which can be signs of nutritional deficiencies.
6. Headaches and Migraines
Fluctuating estrogen levels are a known migraine trigger. For some women, the pill reduces migraines by stabilizing hormones; for others particularly those who experience migraines with aura it can worsen them significantly.
Important safety note: Women who experience migraines with aura (visual disturbances, numbness, or speech changes preceding the headache) are generally advised against using combined estrogen-containing contraceptives due to an increased risk of ischemic stroke. This is one of the few birth control side effects that carries a serious medical risk and should be discussed thoroughly with your provider.
7. Skin Changes: Acne and Beyond
The pill is frequently prescribed specifically to treat acne and for some women, it works beautifully. Pills containing certain progestins (particularly drospirenone, as in Yaz or Yasmin) have anti-androgenic effects that reduce oil production and clear hormonal acne.
But for other women particularly those on progestin-only methods like the mini-pill, the shot, or the implant acne can worsen significantly. Progestins with androgenic activity (like norethindrone or levonorgestrel) can increase oil production and trigger breakouts.
Skin changes after starting birth control are common and are almost always directly related to the specific progestin type in your contraceptive. If your skin has worsened since starting a new method, the progestin type may be the issue not something inherently wrong with you.
8. Weight Changes and Bloating
Weight gain is one of the most commonly reported birth control complaints, yet clinical studies have struggled to confirm a consistent, significant effect across all methods. Here is what the research actually shows:
The shot (Depo-Provera) has the strongest evidence for weight gain studies show an average gain of 5–10 pounds over the first year for some users
The hormonal IUD delivers progestin locally with minimal systemic absorption and is least associated with weight changes
The combined pill may cause water retention and bloating, which some women experience as weight gain even without actual fat gain
The implant has shown modest weight gain in some studies
Bloating, breast tenderness, and fluid retention in the first few months of starting a new hormonal method are common as your body adjusts and often resolve within 2–3 cycles.
9. The Post-Pill Adjustment Period
When you stop taking hormonal birth control especially after years of use your body needs time to recalibrate its own hormone production. This adjustment period can involve:
Post-pill amenorrhea absence of periods for 3–6 months after stopping (sometimes longer)
Hormonal acne flares as androgen levels temporarily rise without the pill's suppressive effects
Mood fluctuations as natural hormone cycling resumes
Changes in discharge and vaginal environment as cervical mucus patterns normalize
Temporary fertility delay particularly with the shot, which can suppress ovulation for up to 12–18 months after the last injection
This adjustment is normal and expected. However, if your period has not returned within 3 months of stopping hormonal birth control, it is worth checking in with your provider to rule out other causes.
The Copper IUD: Non-Hormonal but Not Without Side Effects
For women seeking non-hormonal birth control, the copper IUD (Paragard) is often positioned as the clean, side-effect-free option. And it is true that it contains no hormones. But it is not without its own side effects:
Heavier periods the copper IUD is associated with significantly heavier menstrual bleeding, particularly in the first 3–6 months; for women who already have heavy periods, this is an important consideration
Worsening cramps many women experience significantly more painful periods with the copper IUD
Spotting between periods especially in the adjustment months after insertion
Increased BV risk some research suggests the copper IUD may alter the vaginal environment and increase BV susceptibility, possibly related to changes in uterine fluid
Finding the Right Method for Your Body
Here is the most important thing to take away from this post: there is no single "best" birth control for all women. The right method is the one that works for your body, your health history, your lifestyle, and your goals.
If you are experiencing side effects that are affecting your quality of life your mood, your sex drive, your skin, your vaginal health those concerns are valid and worth addressing. You have options:
Try a different pill formulation with a different progestin type
Switch from a combined method to a progestin-only method, or vice versa
Consider a non-hormonal option like the copper IUD, condoms, or a diaphragm
Ask about the hormonal IUD, which delivers hormones locally with the least systemic effect
Take a break from hormonal birth control entirely and track your natural cycle using fertility awareness methods (with proper education)
The key is to advocate for yourself clearly and specifically. Rather than saying "the pill isn't agreeing with me," walk in with specifics: "Since starting this pill, I have experienced X, Y, and Z. I want to discuss whether a different formulation or method might work better for my body."
When to Call Your Doctor Right Away
Some birth control side effects require immediate medical attention. Seek care urgently if you experience:
Severe chest pain or shortness of breath possible blood clot in the lung
Sudden severe headache, vision changes, weakness on one side of the body, or difficulty speaking possible stroke
Severe abdominal pain possible blood clot in the abdomen or, with an IUD, possible ectopic pregnancy
Leg pain, swelling, or redness possible deep vein thrombosis (DVT)
These serious complications are rare but real and are why women with certain risk factors (smoking, migraines with aura, blood clotting disorders, high blood pressure) need thorough screening before starting estrogen-containing contraceptives.
Frequently Asked Questions
Does birth control cause infertility?
No. For the vast majority of methods, fertility returns quickly after stopping often within the first cycle. The exception is the shot (Depo-Provera), which can delay fertility return for up to 12–18 months. Birth control does not cause permanent infertility.
Can birth control affect my long-term hormone levels?
Research suggests that most hormonal effects of birth control are reversible after stopping. However, some women particularly those who started the pill in adolescence and used it for many years may experience a longer adjustment period as their hypothalamic-pituitary-ovarian axis recalibrates.
Should I take a break from birth control periodically?
There is no medical requirement to take "breaks" from hormonal birth control for safety reasons. However, if you are experiencing side effects, a break can help you determine what is the pill versus what is baseline for your body and gives your microbiome and nutrient levels a chance to normalize.
Can birth control affect my thyroid?
The combined pill can increase levels of thyroid-binding globulin (TBG), which affects how thyroid hormones circulate in the blood. This can alter thyroid test results and may affect thyroid medication dosing in women with hypothyroidism. If you are on thyroid medication and start or stop the pill, let your prescriber know.
Resources & Sources
Skovlund, C.W., et al. (2016). Association of Hormonal Contraception with Depression. JAMA Psychiatry.
Panzer, C., et al. (2006). Impact of oral contraceptives on sex hormone-binding globulin and androgen levels. Journal of Sexual Medicine.
American College of Obstetricians and Gynecologists (ACOG) Hormonal Contraception: acog.org
Centers for Disease Control and Prevention (CDC) U.S. Medical Eligibility Criteria for Contraceptive Use: cdc.gov
Mayo Clinic Birth Control Pill: mayoclinic.org
National Institutes of Health (NIH) Contraception Research: pubmed.ncbi.nlm.nih.gov
Wooltorton, E. (2004). Revisiting the safety of Depo-Provera. Canadian Medical Association Journal.
Has your birth control ever affected your mood, your sex drive, your skin, or your vaginal health? Share in the comments below. This is a no-judgment space for every question.
Author
Becky Freeman is the founder of BVTalks® and Bee Vee Clean. She focuses on women’s intimate health, vaginal microbiome education, and creating practical, easy-to-understand content for everyday care.
Disclaimer: This post is for educational purposes only and is not a substitute for professional medical advice. Always consult your healthcare provider before starting, stopping, or changing any birth control method.